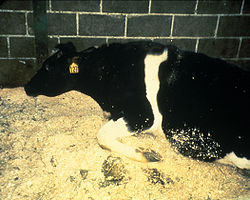
Bovine spongiform encephalopathy
From Wikipedia, the free encyclopedia
Bovine Spongiform Encephalopathy (BSE), commonly known as Mad-Cow Disease (MCD), is a fatal, neurodegenerative disease in cattle, that causes a spongy degeneration in the brain and spinal cord and red eyes. BSE has a long incubation period, about 4 years, usually affecting adult cattle at a peak age onset of four to five years, all breeds being equally susceptible.[1] In the United Kingdom, the country worst affected, more than 179,000 cattle have been infected and 4.4 million slaughtered during the eradication programme.[2]
It is believed by most scientists that the disease may be transmitted to human beings who eat the brain or spinal cord of infected carcasses.[3] In humans, it is known as new variant Creutzfeldt-Jakob disease (vCJD or nvCJD), and by April 2008, it had killed 163 people in Britain, and 37 elsewhere[4] with the number expected to rise because of the disease's long incubation period.[5] Between 460,000 and 482,000 BSE-infected animals had entered the human food chain before controls on high-risk offal were introduced in 1989.[6]
A British inquiry into BSE concluded that the epidemic was caused by cattle, who are normally herbivores, being fed the remains of other cattle in the form of meat and bone meal (MBM), which caused the infectious agent to spread.[7][8] The origin of the disease itself remains unknown. The infectious agent is distinctive for the high temperatures at which it remains viable; this contributed to the spread of the disease in Britain, which had reduced the temperatures used during its rendering process.[7] Another contributory factor was the feeding of infected protein supplements to very young calves.[7][9]
Contents[hide] |
[edit] Infectious agent

The infectious agent in BSE is believed to be a specific type of misfolded protein called a prion. Those prion proteins carry the disease between individuals and cause deterioration of the brain. BSE is a type of transmissible spongiform encephalopathy (TSE).[10] TSEs can arise in animals that carry an allele which causes previously normal protein molecules to contort by themselves from an alpha helical arrangement to a beta pleated sheet, which is the disease-causing shape for the particular protein. Transmission can occur when healthy animals come in contact with tainted tissues from others with the disease. In the brain these proteins cause native cellular prion protein to deform into the infectious state, which then goes on to deform further prion protein in an exponential cascade. This results in protein aggregates, which then form dense plaque fibers, leading to the microscopic appearance of "holes" in the brain, degeneration of physical and mental abilities, and ultimately death.
Different theories exist for the origin of prion proteins in cattle. Two leading theories suggest that it may have jumped species from the disease scrapie in sheep, or that it evolved from a spontaneous form of "mad cow disease" that has been seen occasionally in cattle for many centuries.[11] Publius Flavius Vegetius Renatus records cases of a disease with similar characteristics in the 4th and 5th Century AD.[12] The British Government enquiry took the view the cause was not scrapie as had originally been postulated, and was some event in the 1970s that was not possible to identify.[13]
Not all scientists agree that the danger of contracting the disease warrants taking extreme measures. They stress that human infection by mad cow disease has been statistically very small.[citation needed]
[edit] The BSE epidemic in British cattle
Cattle are normally herbivores. In nature, cattle eat grass. In modern industrial cattle-farming, various commercial feeds are used, which may contain ingredients including antibiotics, hormones, pesticides, fertilizers, and protein supplements. The use of meat and bone meal, produced from the ground and cooked left-overs of the slaughtering process as well as from the cadavers of sick and injured animals such as cattle, sheep, or chickens, as a protein supplement in cattle feed was widespread in Europe prior to about 1987.[citation needed] Worldwide, soya bean meal is the primary plant-based protein supplement fed to cattle. However, soya beans do not grow well in Europe, so cattle raisers throughout Europe turned to the less expensive animal by-product feeds as an alternative. A change to the rendering process in the early 1980s may have resulted in a large increase of the infectious agents in the cattle feed. A contributing factor was suggested to have been a change in British laws that allowed a lower temperature sterilization of the protein meal. While other European countries like Germany required said animal byproducts to undergo a high temperature steam boiling process, this requirement had been eased in Britain as a measure to keep prices competitive. Later the British Inquiry dismissed this theory saying "changes in process could not have been solely responsible for the emergence of BSE, and changes in regulation were not a factor at all."[14]
Following an epizootic of BSE in Britain, 165 people (up until 2007) acquired and died of a disease with similar neurological symptoms subsequently called vCJD, or (new) variant Creutzfeldt-Jakob disease. This is a separate disease from 'classical' Creutzfeldt-Jakob disease, which is not related to BSE and has been known about since the early 1900s. Three cases of vCJD occurred in people who had lived in or visited Britain — one each in Ireland, Canada and the United States. There is also some concern about those who work with (and therefore inhale) cattle meat and bone meal, such as horticulturists, who use it as fertilizer. Up to date statistics on all types of CJD are published by the UK CJD Surveillance Centre in Edinburgh.
For many of the vCJD patients, direct evidence exists that they had consumed tainted beef, and this is assumed to be the mechanism by which all affected individuals contracted it. Disease incidence also appears to correlate with slaughtering practices that led to the mixture of nervous system tissue with hamburger and other beef. It is estimated that 400,000 cattle infected with BSE entered the human food chain in the 1980s. Although the BSE epizootic was eventually brought under control by culling all suspect cattle populations, people are still being diagnosed with vCJD each year (though the number of new cases currently has dropped to fewer than 5 per year). This is attributed to the long incubation period for prion diseases, which are typically measured in years or decades. As a result the full extent of the human vCJD outbreak is still not fully known.
The scientific consensus is that infectious BSE prion material is not destroyed through normal cooking procedures, meaning that contaminated beef foodstuffs prepared "well done" may remain infectious.[15][16]
In 2004 researchers reported evidence of a second contorted shape of prions in a rare minority of diseased cattle. In other words, this implies a second strain of BSE prion. Very little is known about the shape of disease-causing prions, because their insolubility and tendency to clump thwarts application of the detailed measurement techniques of structural biology. But cruder measures yield a "biochemical signature" by which the newly discovered cattle strain appears different from the familiar one, but similar to the clumped prions in humans with traditional CJD Creutzfeldt-Jakob Disease. The finding of a second strain of BSE prion raises the possibility that transmission of BSE to humans has been underestimated, because some of the individuals diagnosed with spontaneous or "sporadic" CJD may have actually contracted the disease from tainted beef. So far nothing is known about the relative transmissibility of the two disease strains of BSE prion.
Alan Colchester, a professor of neurology at the University of Kent, writing in the September 3, 2005 issue of the controversial medical journal, The Lancet, proposed a theory that the most likely initial origin of BSE in Britain was the importation from the Indian subcontinent of bone meal which contained CJD infected human remains.[17] The government of India vehemently responded to the research calling it "Misleading, highly mischievous, a figment of imagination, absurd," further adding that India maintained constant surveillance and had not had a single case of either BSE or vCJD.[18][19] The authors responded in the January 22, 2006 issue of The Lancet that their theory is unprovable only in the same sense as all other BSE origin theories are and that the theory warrants further investigation.[20]
[edit] UK epizootic and UK licensed medicines
During the course of the investigation into the BSE epizootic, an enquiry was also made into the activities of the Department of Health and its Medicines Control Agency. On May 7, 1999, in his written statement number 476 to the BSE Inquiry, David Osborne Hagger reported on behalf of the Medicines Control Agency that in a previous enquiry the Agency had been asked to:
"... identify relevant manufacturers and obtain information about the bovine material contained in children's vaccines, the stocks of these vaccines and how long it would take to switch to other products." It was further reported that the: "... use of bovine insulin in a small group of mainly elderly patients was noted and it was recognised that alternative products for this group were not considered satisfactory." A medicines licensing committee report that same year recommended that: "... no licensing action is required at present in regard to products produced from bovine material or using prepared bovine brain in nutrient media and sourced from outside the United Kingdom, the Channel Isles and the Republic of Ireland provided that the country of origin is known to be free of BSE, has competent veterinary advisers and is known to practise good animal husbandry." In 1990 the British Diabetic Association became concerned regarding the safety of bovine insulin and the government licensing agency assured them that: "... there was no insulin sourced from cattle in the UK or Ireland and that the situation in other countries was being monitored." In 1991 a European Community Commission: "... expressed concerns about the possible transmission of the BSE/scrapie agent to man through use of certain cosmetic treatments." Sources in France reported to the British Medicines Control Agency: "... that there were some licensed surgical sutures derived from French bovine material." Concerns were also raised: "... regarding a possible risk of transmission of the BSE agent in gelatin products."
[edit] Husbandry practices in the United States relating to BSE
Soybean meal is cheap and plentiful in the United States. As a result, the use of animal byproduct feeds was never common, as it was in Europe. However, U.S. regulations only partially prohibit the use of animal byproducts in feed. In 1997, regulations prohibited the feeding of mammalian byproducts to ruminants such as cows and goats. However, the byproducts of ruminants can still be legally fed to pets or other livestock such as pigs and poultry such as chickens. In addition, it is legal for ruminants to be fed byproducts from some of these animals. [2] A proposal to end the use of cow blood, restaurant scraps, and poultry litter (fecal matter, feathers)[21] in January 2004 has yet to be implemented [3], despite the efforts of some advocates of such a policy, who cite the fact that cows are herbivores, and that blood and fecal matter could potentially carry BSE.
In February 2001, the USGAO reported that the FDA, which is responsible for regulating feed, had not adequately policed the various bans. [4] Compliance with the regulations was shown to be extremely poor before the discovery of the Washington cow, but industry representatives report that compliance is now 100%. Even so, critics call the partial prohibitions insufficient. Indeed, US meat producer Creekstone Farms alleges that the USDA is preventing BSE testing from being conducted [5].
Japan was the top importer of U.S. beef, buying 240,000 tons valued at $1.4 billion in 2003. After the discovery of the first case of BSE in the U.S. on December 23, 2003, Japan stopped U.S. beef imports in December 2003. In December 2005, Japan once again allowed imports of U.S. beef, but reinstated its ban in mid-January 2006 after a technical violation of the U.S.-Japan beef import agreement: a vertebral column, which should have been removed prior to shipment, was included in a shipment of veal.
Tokyo yielded to U.S. pressure to resume imports, ignoring consumer worries about the safety of U.S. beef, said Japanese consumer groups. Michiko Kamiyama from Food Safety Citizen Watch said about this: "The government has put priority on the political schedule between the two countries, not on food safety or human health."
Possibly due to pressure from large agribusiness, the United States has drastically cut back on the number of cows inspected for BSE.[22]
65 nations have full or partial restrictions on importing U.S. beef products because of concerns that U.S. testing lacks sufficient rigor. As a result, exports of U.S. beef declined from $3.8 billion in 2003, before the first mad cow was detected in the US, to $1.4 billion in 2005. [22]
On December 31, 2006, Hematech, a biotechnology company based in Sioux Falls, South Dakota, announced that it had used genetic engineering and cloning technology to produce cattle that lacked a necessary gene for prion production - thus theoretically making them immune to BSE.[23]
[edit] BSE statistics by country
| Country | BSE cases | vCJD cases | Country | BSE cases | vCJD cases |
|---|---|---|---|---|---|
| Austria | 5 | 0 | Belgium | 125 | 0 |
| Canada | 10 | 1 | Czech Republic | 9 | 0 |
| Denmark | 15 | 0 | Falkland Islands | 1 | 0 |
| Finland | 1 | 0 | France | 900+ | 11 |
| Germany | 312 | 0 | Greece | 1 | 0 |
| Hong Kong | 2 | 0 | Israel | 1 | 0 |
| Italy | 117 | 1 | Japan | 26 | 1 |
| Liechtenstein | 2 | 0 | Luxembourg | 2 | 1 |
| Netherlands | 75 | 2 | Oman | 2 | 0 |
| Poland | 21 | 0 | Portugal | 875 | 2 |
| Republic of Ireland | 1,353 | 4 | Slovakia | 15 | 0 |
| Slovenia | 7 | 0 | Spain | 412 | 2 |
| Sweden | 1 | 0 | Switzerland | 453 | 0 |
| Thailand | n/a | 2 | United Kingdom | 183,823 | 163 |
| United States | 3 | 3 | Total | 188,535 | 193 (+ 60 results pending) |
The table to the right summarizes reported cases of BSE and of vCJD by country. BSE is the disease in cattle, while vCJD is the disease in people.
The tests used for detecting BSE vary considerably as do the regulations in various jurisdictions for when, and which cattle, must be tested. For instance, in the EU the cattle tested are older (30 months+), while many cattle are slaughtered earlier than that. At the opposite end of the scale, Japan tests all cattle at the time of slaughter. Tests are also difficult as the altered prion protein has very small levels in blood or urine, and no other signal has been found. Newer tests are faster, more sensitive, and cheaper, so it is possible that future figures may be more comprehensive. Even so, currently the only reliable test is examination of tissues during an autopsy.
It is notable that there are no cases reported in Australia, New Zealand and Vanuatu where cattle are mainly fed outside on grass pasture and, mainly in Australia, non-grass feeding is done only as a final finishing process before the animals are processed for meat.
As for vCJD in humans, autopsy tests are not always done and so those figures too are likely to be too low, but probably by a lesser fraction. In the UK anyone with possible vCJD symptoms must be reported to the UK Creutzfeldt-Jakob Disease Surveillance Unit and so it is unlikely that any cases would be missed. In the U.S., the CDC has refused to impose a national requirement that physicians and hospitals report cases of the disease. Instead, the agency relies on other methods, including death certificates and urging physicians to send suspicious cases to the National Prion Disease Pathology Surveillance Center (NPDPSC) at Case Western Reserve University in Cleveland, which is funded by the CDC.
[edit] References
- ^ A Focus on Bovine Spongiform Encephalopathy. Pathogens and Contaminants. Food Safety Research Information Office (November 2007). Retrieved on 2008-04-07.
- ^ Brown, David (2001-06-19). The 'recipe for disaster' that killed 80 and left a £5bn bill. The Daily Telegraph. Retrieved on 2008-04-07.
- ^ Commonly Asked Questions About BSE in Products Regulated by FDA's Center for Food Safety and Applied Nutrition (CFSAN). Center for Food Safety and Applied Nutrition, Food and Drug Administration (2005-09-14). Retrieved on 2008-04-08.
- ^ Variant Creutzfeld-Jakob Disease, Current Data (April 2008). The National Creutzfeldt-Jakob Disease Surveillance Unit (NCJDSU), University of Edinburgh (April 2008). Retrieved on 2008-04-08.
- ^ Creutzfeldt-Jakob Disease Fact Sheet. National Institute of Neurological Disorders and Stroke (2008-02-13). Retrieved on 2008-04-08.
- ^ CJD deaths 'may have peaked'. BBC News (2001-11-23). Retrieved on 2008-04-08.
- ^ a b c "BSE: Disease control & eradication - Causes of BSE", Department for Environment, Food, and Rural Affairs, March 2007.
- ^ "The BSE Inquiry", led by Lord Phillips of Worth Matravers, report published October 2000.
- ^ Harden, Blaine (2003-12-28). Supplements used in factory farming can spread disease. The Washington Post. Retrieved on 2008-04-08.
- ^ Bovine Spongiform Encephalopaphy: An Overview (PDF). Animal and Plant Health Inspection Service, United States Department of Agriculture (December 2006). Retrieved on 2008-04-08.
- ^ New Scientist, 17 March 2007, p 11
- ^ Digesta Artis Mulomedicinae, Publius Flavius Vegetius Renatus
- ^ Vol.1 - Executive Summary of the Report of the Inquiry
- ^ Vol.2 - 3. The nature and cause of BSE
- ^ http://www.mayoclinic.com/health/mad-cow-disease/ID00012
- ^ Bovine Spongiform Encephalopathy - "Mad Cow Disease". Fact Sheets. Food Safety and Inspection Service (March 2005). Retrieved on 2008-04-08.
- ^ http://www.gaudiyadiscussions.com/topic_4034.html
- ^ India dismisses Lancet's mad cow-India-The Times of India
- ^ The World Today - New theory traces mad cow disease to animal feed exported from India
- ^ Elsevier
- ^ The term "chicken litter" also includes spilled chicken feed as well as fecal matter and feathers. It is still legal in the United States to use ruminant protein to feed chickens. Thus, ruminant protein can get into the food chain of cattle in this round about way.
- ^ a b USA Today, August 3, 2006, archived at [1]
- ^ Weiss, Rick. "Scientists Announce Mad Cow Breakthrough", The Washington Post, 2007-01-01. Retrieved on 2007-01-01.
[edit] External links
Government
- APHIS - BSE Information - U.S. Department of Agriculture
- Canadian BSE FAQs - Canadian Food Inspection Agency
- BSE Homepage - Department for Environment, Food and Rural Affairs (UK)
- UK government inquiry into BSE from discovery to 1996
- UK Creutzfeldt-Jakob Disease Surveillance Unit
- British Medicines Control Agency statement PDF - (Excerpts cited above.)
- BSE Resources - Food Safety.gov
- Impact of BSE on U.S. Economy - Economic Research Service
- Mad Cow FAQs - Massachusetts Public Health
- BSE (Mad Cow Disease) - Health Canada
- List of prohibited substances in ruminant feed - U.S. Code of Federal Regulations
- Bovine Spongiform Encephalopathy in North America - enumeration of reported cattle incidents
Consumer/health groups
- HowStuffWorks Craig C. Freudenrich, Ph.D.
- Mad Cow Disease news and information - Organic Consumers Association
- Pediatrician's evaluation of BSE risk- About.com
- Mad Cow information - Bureau for National Affairs
- BSE FAQs - International Food Information Council
- Mad Cow USA - Center for Media and Democracy
- Choosing Safer Beef to Eat - Center for Science in the Public Interest
Science/research
- BSE and blood transfusion (The Lancet - Vol. 368, Issue 9552, 09 December 2006, Pages 2061-2067)
- Scientific American - Article from 2004
- Mad Cow Information - North Dakota State University
- BSE Information Center - Iowa State University
- The Origins of BSE - Mark Purdey
Beef/cattle industry
- BSE News & Information - American Association of Meat Processors
- Livestock Feed Industry News - American Feed Industry Association
- BSE: environmental causation?